The University of British Columbia Faculty of Medicine’s Division of Rural Continuing Professional Development (Rural CPD) supports rural health care providers to build relationships and engage in learning activities “closer to home,” in their usual context of health care delivery in rural, remote, and Indigenous communities.
The goal of Rural CPD is to cultivate strong relationships with, and meet the needs of, partners, project stakeholders, and rural healthcare practitioners. With its shared commitment to improving the health of people and communities in rural British Columbia (BC), Rural CPD operates in partnership with the Rural Coordination Centre of BC (RCCbc) to deliver impactful educational opportunities, offering rurally-specific CPD programs that are community-based, interprofessional, interactive, and practical. In addition to multi-modal learning opportunities, Rural CPD conducts a variety of research and evaluation activities related to the provision of medicine in rural BC. Rural CPD is supported and funded by RCCbc through the Joint Standing Committee on Rural Issues.

Explore the Numbers
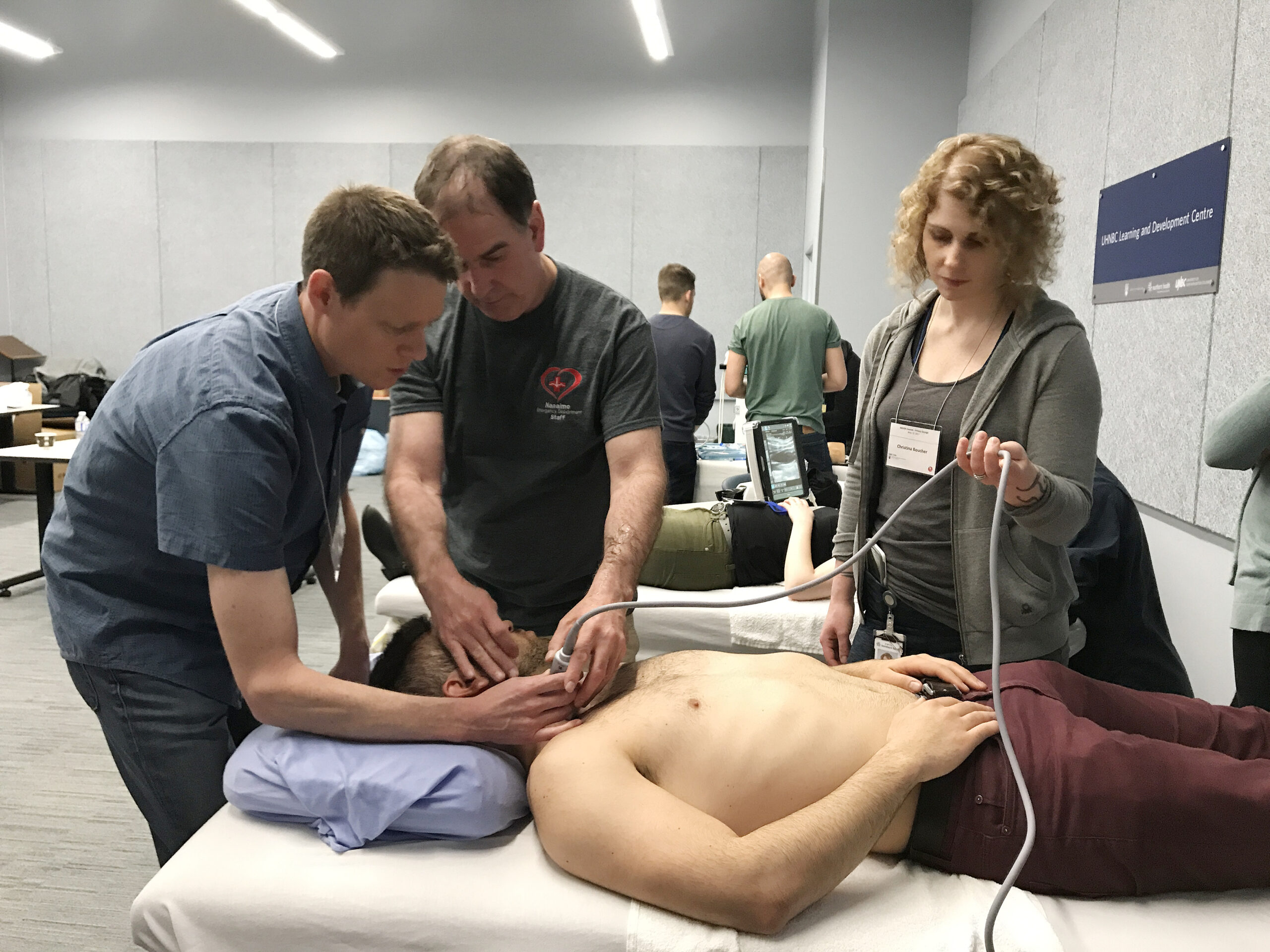
21 Ultrasound Education Days
Hands on Ultrasound Education course days took place in 9 communities, reaching 165 participants in majority RSA A communities.
10 Rural PoCUS Rounds
These Rural Point of Care Ultrasound (PoCUS) Rounds sessions, reached 450 participants.
40 RTVS Virtual Simulations
Topics included pediatric head trauma, postpartum hemorrhage, and pneumosepsis.
543 Rural Rounds Participants
A series of 10 Rural Rounds sessions reached 543 participants.
Making a Difference
Just one-month post course, a participant from the Hands on Ultrasound Education course for Obstetrics reflected on their progress: “I have done a bunch of viability scans – 3 that confirmed viability (especially good for one mama who had 5 losses last year).”
Additional feedback from participants of the Hands on Ultrasound Education (HOUSE) course reinforces the value of the program for rural practitioners:
Those participating in the Rural Rounds, Pediatric DERMES and Coaching and Mentoring Program highlighted the benefits of educational opportunities catered directly towards healthcare providers in rural communities:
Plans for the Future
UBC Rural CPD is committed to supporting the learning needs of physicians and other health care providers who practice in rural, remote, and Indigenous communities in British Columbia. The program demonstrates that through community-based, interprofessional, collaborative, and practical CPD, rural health care providers can be supported to deliver safe and effective health care to rural British Columbians. This is achieved through strong relationships with partners, collaborators, and team members as well as strong pedagogical approaches to education and professional development.
Looking forward, the team will keep investing in relationships with partners, collaborators and rural physician learners. They will continue to bring an equity lens to all that they do to ensure that rural providers who need it the most are supported.
Team Members
Click on a team member to explore which other projects they have contributed to in the past year.

Dana Hubler
Medical Director, Rural Continuing Professional Development
Dana Hubler’s Projects: Annual Reports

Laura Beamish
Senior Manager, Rural Program, Rural CPD (On leave)